How to Effectively Dispense Compression Therapy In-Office
Dispensing compression systems from my office is extremely rewarding. Patients enjoy being handed the product they need, rather than having to hunt for it in their community. Specifically, patients in need of compression therapy find that not all compression garments are right for them. Oftentimes, these patients enjoy the ease of application and adjustment that the EXTREMIT-EASE® Compression Garment offers, which I find to be superior to other options on the market. Dispensing EXTREMIT-EASE can also be a profitable endeavor for your practice if all the proper guidelines are followed.
Guidelines
Gradient compression wraps are considered “surgical dressings” and, as such, fall under the DMEMAC Surgical Dressing Local Coverage Determination. Therefore, in order for a compression garment to be a covered service, the patient must have a qualifying wound that was either surgically created or debrided. Compression garments covered under DMEMAC can serve as either a primary dressing or secondary dressing. In the case that is serves as a secondary dressing, a qualifying primary dressing may also be dispensed at the same time. One EXTREMIT-EASE garment is covered by the DMEMACs once per 6 moths per leg. If a replacement garment is dispensed, it is only a candidate for reimbursement if a qualifying wound is still present.
Coding
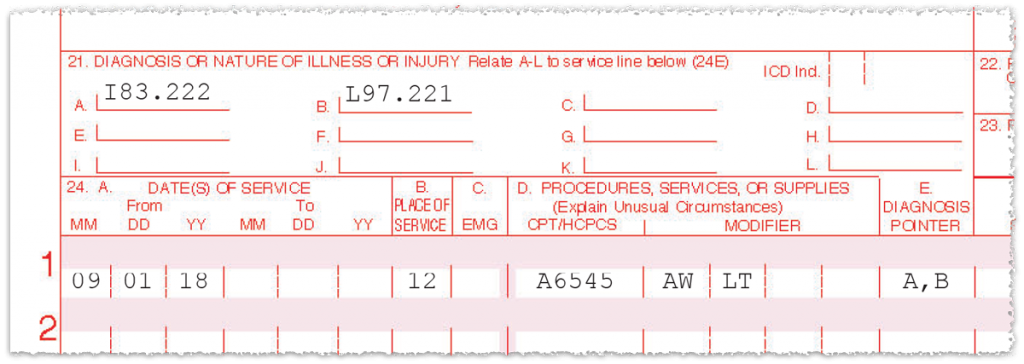
The PDAC-approved HCPCS code for EXTREMIT-EASE is A6545 (Gradient compression wrap, non-elastic below knee, 30-50 mm hg, each). This should be place on one lime of the claim form with both an AW modifier and either an RT or LT modifier, whichever is appropriate for the extremity on which the garment will be used. The AW modifier is not used often but is required with A6545. If bilateral garments are dispensed, one unit of A6545 should be listed on two different claim lines, AW modifier appended to both, and RT modifier for one and LT modifier for the other.

Not Covered
If a qualifying wound is not presented, the AW modifier doesn’t apply, so a patient may choose to pay out of pocket for their garment(s). When this occurs, we may choose to charge the patient what we feel is appropriate. Patients often choose to do this after their wound is healed as they enjoy using the garments to prevent recurrence. I also frequently see patients enjoying the garment so much on the limb with the qualifying wound, that they choose to purchase a second garment for the other leg!
In Conclusion
Following these coding and compliance guidelines is an important aspect of dispensing compression garments. With the proper implementation, dispensing the EXTEMIT-EASE Compression Garment can be extremely rewarding for our practices.
DISCLAIMER: The information provided here is intended to educate health care providers regarding compliance for ICD, CPT, and HCPCS coding. The information provided does not guarantee reimbursement and is accurate to the best of our knowledge at the time of this publication. Coding guidelines can change and we encourage you to stay up to date. The existence of a code does not guarantee payment.

Dr. Jeffrey D. Lehrman, DPM, FASPS, MAPWCA, CPC, CPMA
Dr. Lehrman is a podiatrist practicing in Fort Collins, CO and operates Lehrman Consulting, LLC which provides consultation services regarding coding, compliance and documentation. Dr. Lehrman is a Certified Professional Coder and Certified Professional Medical Auditor. He serves as a staff liaison at the AMA CPT® Editorial Panel meetings where CPT codes are created, edited, and deleted. He is a Diplomate of the American Board of Foot and Ankle Surgery, Fellow of the American Society of Podiatric Surgeons, and is recognized as a “Master” by the American Professional Wound Care Association. Dr Lehrman is a Fellow of the American Academy of Podiatric Practice Management, Past Director of the American Professional Wound Care Association Board of Directors, and is a Past Chairman of the Board of the American Society of Podiatric Surgeons. Dr. Lehrman is also on the editorial advisory board of the journal WOUNDS.